Comorbid substance use disorders and mental health disorders among New Zealand prisoners
Jill Bowman
Principal Research Adviser, Department of Corrections
Author biography:
Jill joined the Department of Corrections’ Research and Analysis Team in 2010. She manages a variety of research and evaluation projects, and has a particular interest in desistance, employment outcomes of released prisoners, how probation officers work with offenders and the needs of female offenders. As well as working for Corrections, she volunteers at Arohata Prison, teaching quilting to the women in the Drug Treatment Unit.
Introduction
A 1999 study of New Zealand prisoners (Department of Corrections, 1999) showed that up to 70% have drug and/or alcohol problems, and a significant proportion have various mental health issues. However, the prevalence of comorbid substance abuse and mental health disorders (which overseas studies have identified as significant amongst prisoners) has not previously been investigated.
Following a successful application to the Government’s Proceeds of Crime fund under the Methamphetamine Action Plan, the Department contracted Auckland-based National Research Bureau (NRB) to interview prisoners about substance use and mental health problems. Over 1,200 prisoners were interviewed in 13 prisons between March and July 2015 using two tools: the World Health Organisation’s Composite International Diagnostic Interview (CIDI) and the Personality Diagnostic Questionnaire (PDQ).
An Australian research consortium including CGA Consulting and researchers affiliated to the University of New South Wales analysed the data collected, and produced a report detailing the findings (Indig, Gear & Wilhelm et al, 2016).
This article summarises significant findings from the study. The full report is available on the Department of Corrections’ website.
Methodology
An earlier Practice article by the author (Bowman, 2015) described how the research was carried out. However, to understand the results, it is worth repeating two context-related caveats here.
The sample of 1,209 prisoners who were interviewed for the study comprised prisoners who had either been sentenced within the last three months or who were remand-convicted prisoners. It was important to restrict participants to newly sentenced prisoners to ensure that the responses to questions about mental health or substance use over the last 12 months were based on prisoners’ experiences while in the community. To reinforce this, interviewers reminded prisoners that their responses should reflect the period before their admission to prison.
A second caveat is the small sample sizes of some groups, which means that some results should be read with caution. For example, although small numbers of prisoners aged over 65 took part in the survey, age breakdowns including this sub-group were retained to enable comparisons with the 2006 New Zealand Mental Health Survey (Oakley Browne, Wells & Scott, 2006).
Results of the study
The study assessed prisoners’ experiences of the following disorders over the preceding 12 months and over their lifetimes: anxiety, mood, substance use, eating, and personality, as well as for symptoms of psychosis, psychological distress and suicidal behaviours. Respondents were also asked whether they had received mental health treatment in the past year.
Where possible, comparisons were made with the 2006 New Zealand Mental Health Survey (Oakley Browne et al, 2006), with the 2013/14 New Zealand Health Survey for psychological distress (Ministry of Health, 2014), and also with the 1999 National Study of Psychiatric Morbidity in New Zealand Prisons (Department of Corrections, 1999).
Results showed, not surprisingly, that prisoners had considerably more issues with substance abuse than the general population, but also that their mental health was significantly worse. Nearly all prisoners (91%) had been diagnosed with either a substance use disorder or a mental health disorder over their lifetime. Over the last 12 months, almost two-thirds of prisoners had been diagnosed with either of these disorders, and this was three times higher than the general population. Female prisoners were much more likely than male prisoners to have been diagnosed with either disorder over the last year.
Figure 1:
Prevalence of a substance use disorder or a mental health disorder
| 12-month diagnosis | Lifetime diagnosis | |
|---|---|---|
| Any substance use disorder | 47 | 87 |
| Any anxiety disorder | 23 | 30 |
| Any mood disorder | 24 | 32 |
| Any mental disorder (includes any mood, anxiety, substance or eating disorder) | 62 | 91 |
Substance use disorder
There is a strong correlation between offending and substance disorders (Young, Wells & Gudjonsson, 2011) and all substance disorders were higher among prisoners than the general population. In fact, the greatest difference between prisoners and the general population for all disorders assessed was for substance use disorders. Questions about substance use disorders covered drug abuse and dependence, and alcohol abuse and dependence. Drug types considered were club drugs, cocaine, hallucinogens, inhalants, marijuana, opioids, painkillers, sedatives and stimulants.
Almost half of all prisoners had had a substance use disorder over the previous 12 months and, over their lifetime, 87% of prisoners had a substance use disorder. These were 13 times and seven times respectively higher than in the general population.
Table 1:
Substance use disorders summary, 2015 prisoner population.
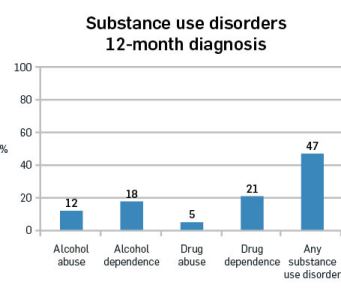
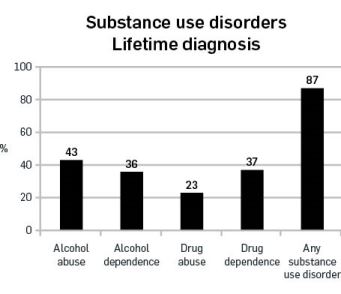
Simply put, alcohol/drug abuse reflects “too much, too often” and dependence is the inability to quit.
The highest difference between the prisoner and general populations for any substance use disorder was for drug dependence, where prisoners were 30 times more likely than the general population to have a 12-month drug dependence diagnosis.
The lifetime findings were similar to the 1999 New Zealand Prisoner Mental Health Study (Department of Corrections, 1999). Alcohol abuse was 43% in 2015 (compared to 39% in the 1999 study), alcohol dependence was 36% in both studies, and any substance abuse disorder was 87% in 2015 (compared to 83%). Drug use was not comparable between the two surveys. However, of note, was the increase in the prevalence of stimulant abuse and dependence combined between the two studies, from 4% in 1999 to 38% in 2015. The more recent rates almost certainly relate predominantly to the drug methamphetamine.
Female prisoners had a higher 12-month and lifetime prevalence of both alcohol and drug dependence than men, but male prisoners had a higher prevalence of alcohol and drug abuse. Whereas females had a higher prevalence of any substance disorder over the last year, males had a higher lifetime prevalence.
Both 12-month and lifetime substance use disorders decrease with age in the general population. While the overall 12-month and life-time diagnoses for prisoners are consistent with this pattern, there is more variability for individual disorders.
Pacific prisoners had the highest prevalence of any substance use disorder (both 12-month and lifetime), with the highest prevalence of alcohol disorders but the lowest prevalence of drug disorders. European prisoners had the lowest prevalence of substance use disorders.
Anxiety disorders
Anxiety disorders covered generalised anxiety disorders, panic disorder and post-traumatic stress disorder. The study did not measure a number of anxiety disorders included in the NZ general population survey: agoraphobia without panic disorder, specific phobia, social phobia and obsessive compulsive disorder.
Five percent of prisoners had a 12-month diagnosis of a generalised anxiety disorder (compared with 2% of the general population), and 9% had a lifetime diagnosis (compared with 6% of the population).
Panic disorder was twice as common among prisoners as in the general population for both the lifetime and 12-month diagnosis. Panic disorder was more prevalent in male than female prisoners, while the reverse was found in the general population.
Nearly a quarter of prisoners had a lifetime diagnosis of post-traumatic stress disorder, which was four times higher than the general population.
The lifetime prevalence of generalised anxiety disorder had increased from 1% in the 1999 New Zealand Prisoner Mental Health Study to nearly 9%, while the lifetime prevalence of panic disorder had increased from nearly 2% to nearly 6%. However, the lifetime prevalence of post-traumatic stress disorder was similar (23% in 1999 and 24% in 2015).
Mood disorders
Mood disorders included bipolar disorder, dysthymia, and major depressive disorder.
Prisoners had a higher prevalence of mood disorders than the general population with 24% of prisoners having a 12-month diagnosis compared with 8% of the general population, and 32% having a lifetime diagnosis compared with 20% of the population. The lifetime prevalence of major depressive disorder decreased slightly (from 23% to 21%) between the 1999 and 2015 prisoner studies, while the lifetime prevalence of bipolar disorder increased from 2% to 11% and dysthymia increased from 1% to 5%.
Female prisoners had a higher prevalence than male prisoners of all mood disorders (both 12-month and lifetime) except bipolar disorder, which was significantly higher among men.
Māori prisoners had the lowest rate of lifetime diagnosis of major depressive disorder, but in the general population they had the highest rate.
Comorbidity
The findings showed that 42% of prisoners had had a co-occurrence of a mental health disorder and a substance disorder over their lifetime. Over a 12-month period, the prevalence of comorbidity in prisoners was 20%.
| 12-month diagnosis | Lifetime diagnosis | |
|---|---|---|
| Any comorbidity | 20 | 42 |
Comorbidity was higher among females than men and comorbidity peaked in the 25-44 year age group, where nearly half had a lifetime diagnosis.
Comorbidity was highest among prisoners of European descent. While prisoners diagnosed with drug dependence had the highest rate of comorbidity in the last 12 months, prisoners diagnosed with alcohol dependence had the highest rate of comorbidity.
Multiple disorders
As well as identifying the prevalence of co-existing mental health and substance use disorders, the analysis also included the prevalence of multiple disorders. This could include more than one mental health disorder or more than one substance disorder and could also include multiple mental health and substance disorders.
Results showed that 17% of prisoners had a 12-month diagnosis of two disorders and 14% had a diagnosis of three or more disorders. Prisoners were nearly four times more likely than the general population to have two or more 12-month diagnoses (31% compared to 8%). Over their lifetime, 30% of prisoners had a diagnosis of two disorders and 35% had a diagnosis of three or more disorders. This was three times higher than in the general population.
Women were more likely than men, in both the prisoner and general population samples, to have multiple disorders.
Figure 3:
Prevalence of multiple disorders
| 12-month diagnosis | Lifetime diagnosis | |
|---|---|---|
| Two or more disorders | 31 | 66 |
Personality disorders
Almost a third of prisoners were found to have a clinically significant personality disorder. This compares with the 1999 New Zealand Prisoner Mental Health Study which found around 60% prevalence of a personality disorder among prisoners. The most common personality disorders were paranoid (15%), antisocial (11%), obsessive compulsive (11%) and borderline (10%). It is possible that observed prevalence of paranoid personality disorder was related to prisoners’ drug use histories.
Men had a higher prevalence of all personality disorders than women, with the exception of schizoid personality disorders (5% in women and 4% in men).
Suicidal behaviours
Suicide is a major cause of death among people with a mental illness (Larney, Topp, Indig, O’Driscoll & Greenberg, 2012; Butler et al, 2006). Unsurprisingly, given their higher prevalence of mental disorders, prisoners were twice as likely as people in the general population to have ever thought about suicide and were four times as likely to have ever attempted suicide.
Consistent with the general population, female prisoners had higher rates of suicidal behaviours than men. However, whereas 12-month and lifetime suicidal behaviours declined steeply with age in the general population, they remained high across all age groups for prisoners. Prisoners of European descent had higher rates of suicidal behaviours than Mäori or Pacific peoples. Prisoners with anxiety disorders had the highest rate of suicidal behaviours.
Mental health treatment
Unexpectedly, findings showed that access to mental health treatment in the last year by prisoners with a 12-month mood disorder diagnosis (58%) was similar to that of the general population (55%). Female prisoners were more likely than male prisoners to access mental health services.
Summary
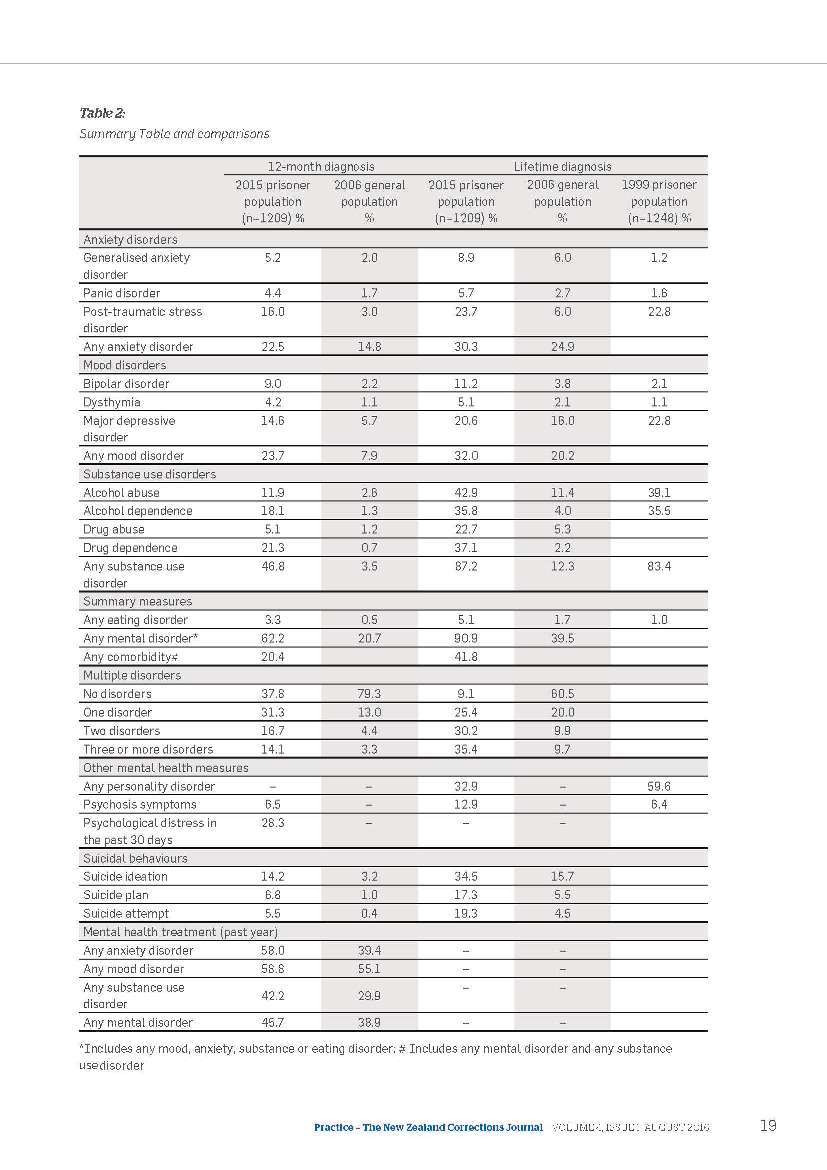
The following table summarises the findings from the study and compares these with the results of the 2006 New Zealand Mental Health Survey and the 1999 National Study of Psychiatric Morbidity in New Zealand Prisons.
Table 2:
Summary Table and comparisons
Generalisability of the study findings
Results were weighted to reflect the prison population by age, gender, and ethnicity as at 17 May 2015, which was around the middle of the interview period. The study sample included a higher proportion of women and younger people relative to proportions commonly observed within the total prisoner population.
Conclusion
Understanding the mental health of prisoners is crucial to being able to provide the best possible care while they are in custody. The information generated by this study will enable Corrections to design and deliver integrated and effective treatment to meet the needs of prisoners with particular health issues.
References
Bowman, J. (2015) Co-morbidity research – Part one. Practice, The New Zealand Corrections Journal, Vol 3, Issue 2, 33 – 34. Department of Corrections
Butler, T., Andrews, G., Allnutt, S., Sakashita, C., Smith, N.E., and Basson, J. (2006). Mental disorders in Australian prisoners: a comparison with a community sample. Australia New Zealand Journal of Psychiatry, issue 40: 272-6.
Indig, D., Gear, C. and Wilhelm, K., (2016) Comorbid substance use disorders and mental health disorders among New Zealand prisoners, Department of Corrections, 2016.
Larney. S., Topp, L., Indig, D., O’Driscoll, C., and Greenberg, D. (2012) A cross-sectional survey of prevalence and correlates of suicidal ideation and suicide attempts among prisoners in New South Wales, Australia. BMC Public Health; Vol 12, Issue 14, 1-14.
Department of Corrections (1999) The National Study of Psychiatric Morbidity in New Zealand Prisons. Department of Corrections
Ministry of Health (2014) Annual update of key results 2013/14: New Zealand Health Survey. Wellington: Ministry of Health.
Oakley Browne, M.A., Wells, J.E., and Scott, K.M. (eds). (2006) Te Rau Hinengaro: The New Zealand Mental Health Survey. Wellington: Ministry of Health.
Young, S., Wells, J. and Gudjonsson, G.H., (2011) Predictors of offending among prisoners: the role of attention-deficit hyperactivity disorder and substance use. Journal of Psychopharmacology, Vol 25, Issue 11, 1524-32.

